The way we act and react is often informed by our past—specifically, by good or bad experiences that help us project what may transpire in the future. A classic example is the Russian psychologist who rang a bell before feeding his dog—eventually the dog learned to salivate at the sound even in the absence of dinner.
But Pavlov’s story tends to glaze over an important factor in this behavioral equation. Today’s neuroscientists have reasons to suspect that associative learning isn’t merely the outcome of a cue being linked to a reward—the order of these events matters, too.
Consider a scenario where the bell normally rings after, not before, the arrival of dog biscuits. To the canine diner, the sound won’t then represent bliss, but the end of bliss; and it will presumably produce memories of sadness rather than of appetite. All of which suggests that the brain doesn’t just file experiences of different kinds in its memory bank—it somehow assigns time stamps to these experiences as well.
Time is a weird thing from a biological perspective, far more abstract than sounds or objects. You can’t see, hear, touch, or taste it, yet the brain seems quite capable of tracking it. Precisely how this chronicling occurs in the context of learning is something that researchers in the lab of Vanessa Ruta, the Gabrielle H. Reem and Herbert J. Kayden Associate Professor, are very keen to understand.
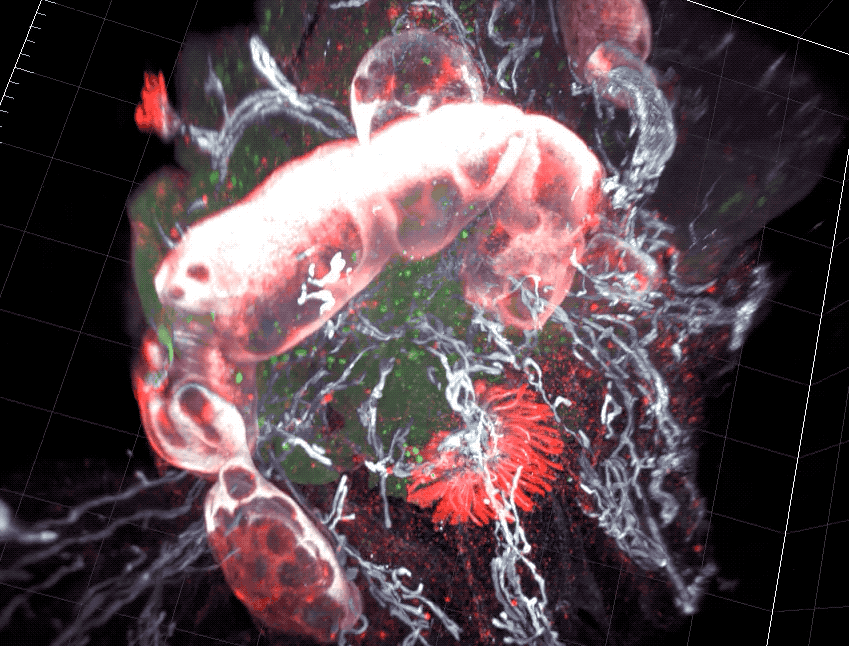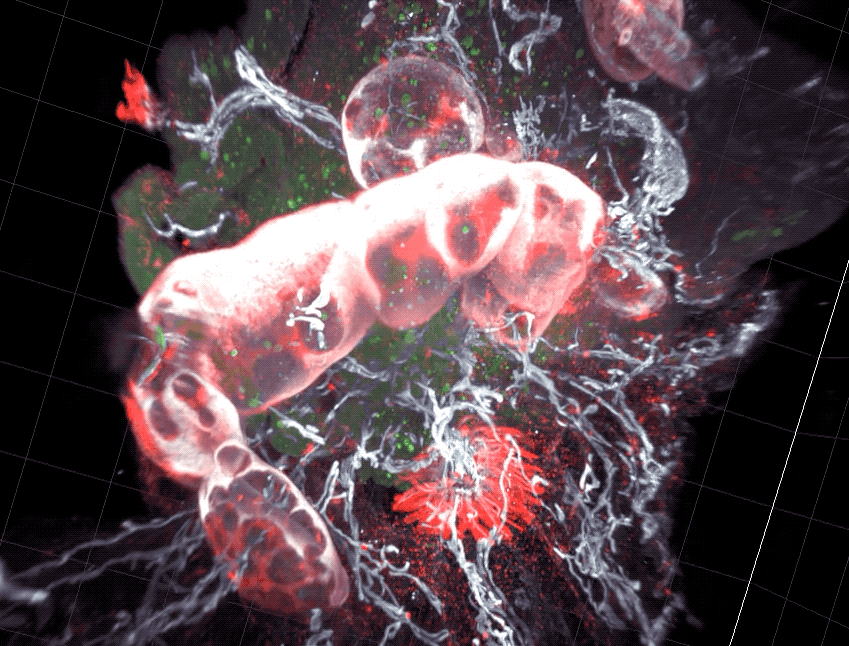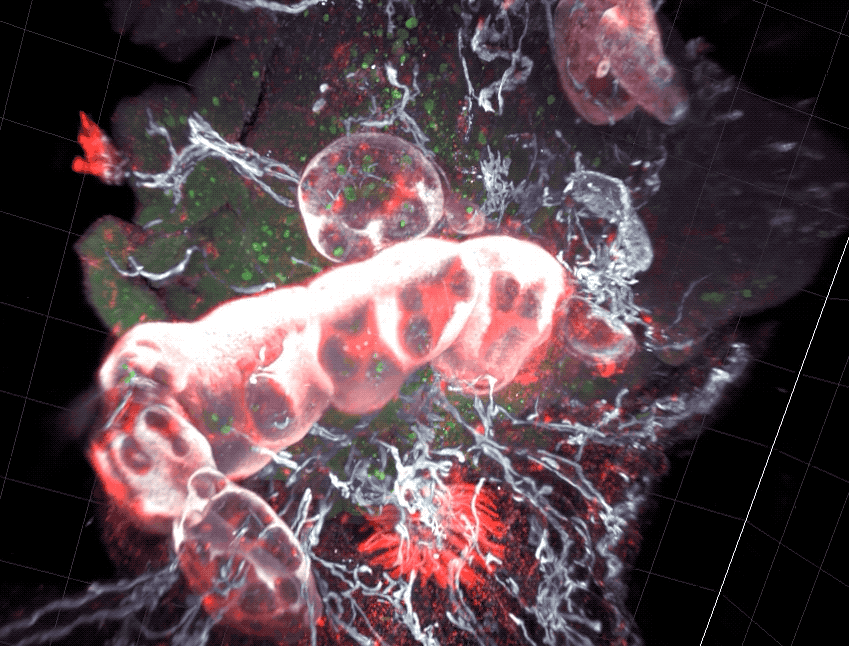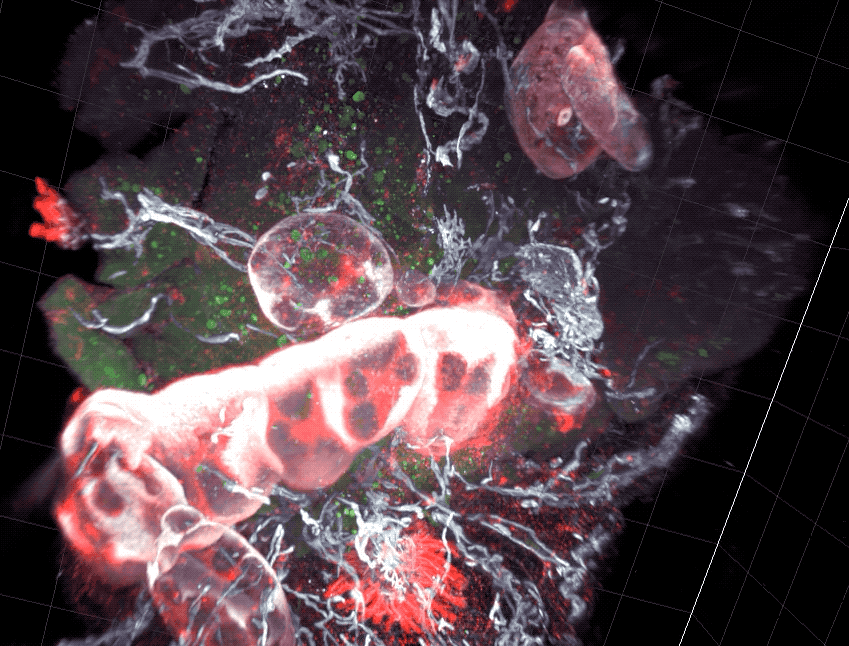
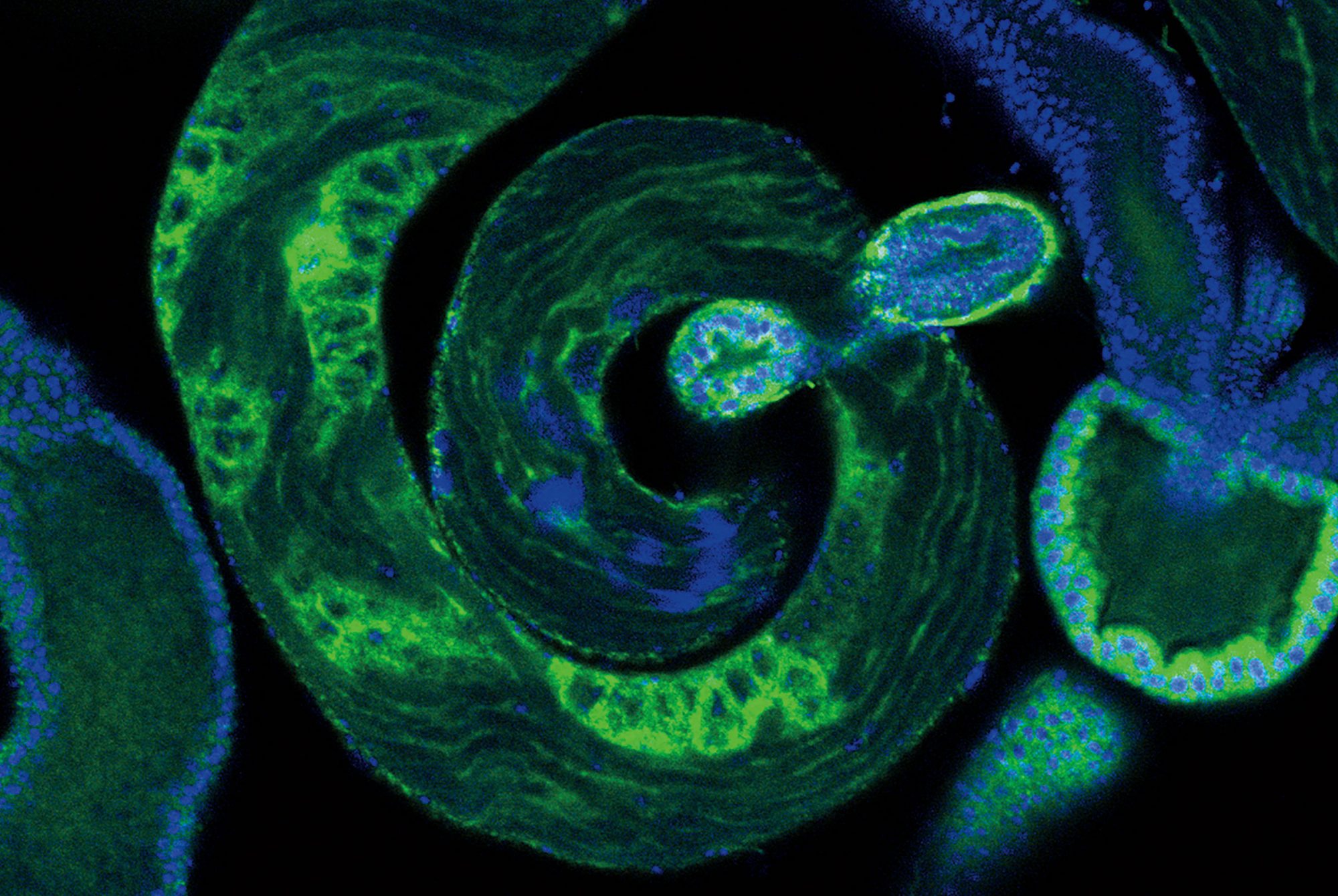
The lab doesn’t have much faith in the dog as a model system, however. For these scientists, man’s best friend is Drosophila melanogaster, the humble fruit fly. Recently, Ruta’s team set up a modern version of Pavlov’s experiment in which they exposed flies to an odor rather than to a sound; and instead of rewarding the animals with a treat, they used optogenetic technology to directly stimulate reward-signaling neurons in the flies’ brains.
The results were clear. When the flies were given a reward signal immediately after receiving a puff of the smell, they became attracted to that scent; but when the reward came before the smell, they shunned it instead. “The difference in time is only one or two seconds, yet the flies form completely opposing associations,” says graduate fellow Annie Handler.
She and her colleagues identified a set of brain cells whose activation enables the fly to know the sequence of events. In addition, they found that flies that had learned to covet the smell could quickly be retrained to detest it, and vice versa. In other words, flies are like us in that their memories are not set in stone.
“There are so many things that we could remember on a daily basis, so we hold on to the memories that turn out to be predictive; and we toss out associations that are incorrect or irrelevant,” says Ruta. “When you live in a dynamic environment—which both flies and humans do—that seems like a very good strategy.”